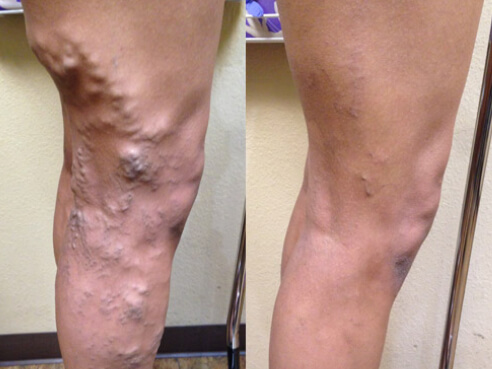
There is no reliable way to confirm deep vein thrombosis at home. While symptoms such as swelling, calf pain, or warmth may raise suspicion, only
Overview
Deep vein thrombosis (DVT) is a serious condition that occurs when a blood clot forms in a deep vein, most commonly in the legs. While some cases develop noticeable symptoms, others may go undetected until complications arise. Although DVT can affect anyone, certain factors significantly increase the risk. Early detection and timely treatment are critical in preventing complications such as pulmonary embolism, a potentially life-threatening condition that occurs when a clot travels to the lungs.
Understanding the causes, warning signs, and risks of DVT can help you recognize when medical attention is necessary.
What Is Deep Vein Thrombosis?
Deep vein thrombosis develops when a blood clot forms in one of the deep veins, usually in the lower leg, thigh, or pelvis. Unlike superficial clots that occur closer to the skin’s surface, deep clots pose greater danger because they can break loose and travel through the bloodstream.
Blood clots form when normal circulation is disrupted. Healthy blood flow keeps moving blood smoothly through the veins. When the flow slows down or blood becomes more prone to clotting, a thrombus (clot) can develop.
What Causes Deep Vein Thrombosis?
DVT typically develops due to one or more of the following factors:
1. Prolonged Immobility
Sitting or lying still for extended periods, such as during long flights, car rides, or bed rest after surgery, can slow blood flow in the deep veins of the legs. When blood circulation becomes sluggish, it increases the likelihood of clot formation, raising the risk of deep vein thrombosis.
2. Injury or Surgery
Damage to the veins caused by surgery, fractures, or trauma can trigger clot formation as part of the body’s natural healing response.
3. Medical Conditions
Certain conditions, including cancer, heart disease, or inherited clotting disorders, increase the likelihood of abnormal clot formation.
4. Hormonal Factors
Birth control pills, hormone replacement therapy, and pregnancy can raise clotting risk due to hormonal changes that affect how blood clots.
5. Obesity and Smoking
Both obesity and smoking impair circulation and increase clotting tendencies, contributing to DVT risk.
Warning Signs of Deep Vein Thrombosis
DVT symptoms can range from mild to severe. Common warning signs include:
- Swelling in one leg (rarely both)
- Pain or tenderness, often starting in the calf
- Warmth in the affected area
- Red or discolored skin
- Leg fatigue or heaviness
The pain may feel like cramping or soreness that does not improve with rest. Swelling can develop gradually or appear suddenly. The affected area may also feel firm to the touch.
Symptoms typically affect only one leg. If both legs are swollen, another condition may be responsible. If symptoms worsen or are accompanied by shortness of breath or chest pain, seek immediate medical attention.
How Serious Is DVT?
Deep vein thrombosis can become life-threatening if part of the clot breaks loose and travels to the lungs, causing a pulmonary embolism (PE). Symptoms of PE may include sudden shortness of breath, sharp chest pain that worsens with breathing, a rapid heartbeat, dizziness, or coughing up blood.
Without proper treatment, DVT can also lead to post-thrombotic syndrome, a long-term condition characterized by chronic leg pain, swelling, skin changes, and, in severe cases, ulcers.
Early diagnosis and appropriate treatment significantly reduce the risk of these serious complications.
How Is DVT Diagnosed?
If DVT is suspected, medical evaluation is essential. A physician may use:
- Ultrasound imaging
- Blood tests (D-dimer)
- Venography (in rare cases)
Often, a duplex ultrasound is the first and most common test used because it can visualize blood flow and detect clots in deep veins. A D-dimer blood test may help rule out the presence of an abnormal clot, particularly in individuals considered to be at low risk.
Your doctor will also review your medical history, risk factors, and symptoms before confirming a diagnosis. Self-diagnosis is unreliable, as DVT symptoms can resemble other conditions. A professional assessment ensures accurate identification and timely, appropriate treatment to reduce the risk of complications.
Can DVT Go Unnoticed?
Yes, deep vein thrombosis can sometimes develop without clear or noticeable symptoms. This is often referred to as “silent” DVT. Because symptoms may be mild or absent, awareness of personal risk factors is especially important.
In some cases, the first noticeable sign may be a pulmonary embolism, which occurs when part of the clot travels to the lungs. For this reason, individuals at higher risk, such as those recovering from surgery, experiencing prolonged immobility, or traveling long distances, should take preventive measures and seek medical evaluation if concerns arise.
Preventing Deep Vein Thrombosis
Prevention focuses on maintaining healthy circulation. Helpful strategies include:
- Staying active and avoiding prolonged sitting
- Taking breaks to stretch during travel
- Wearing compression stockings (as recommended by your doctor)
- Maintaining a healthy weight
- Staying hydrated
- Quitting smoking
After surgery or hospitalization, doctors may prescribe blood thinners to reduce clotting risk.
When to Seek Medical Attention
Seek immediate medical care if you experience:
- Sudden leg swelling
- Persistent calf pain
- Shortness of breath
- Chest pain
- Unexplained rapid heart rate
Early intervention can prevent complications and improve outcomes.
Final Thoughts
Deep vein thrombosis is a serious but treatable condition. Recognizing risk factors and symptoms is essential for timely care. While some cases develop gradually, others can escalate quickly if left untreated.
If you notice warning signs or have concerns about circulation or risk of clots, a professional evaluation can provide clarity and peace of mind. For reliable information, expert guidance, and support related to vein health, visit Vein Specialty Medical Clinic or call (408) 378-3467 to learn more about your options.
This blog has been reviewed by Dr. Khalil Fattahi, MD, ABVLM, Founder of Vein Specialty Medical Clinic and inventor of Foam Washout Sclerotherapy for varicose veins. Board-certified by the American Board of Venous & Lymphatic Medicine and a registered phlebology sonographer, Dr. Fattahi brings over 35 years of expertise in phlebology to his patients. He has performed more than 70,000 sclerotherapy procedures and 10,000+ endovenous ablations, the most of any phlebologist in California, and has presented at numerous national and international phlebology conferences, making him one of the foremost authorities on venous and vascular medicine in the United States.
Frequently asked questions
What is the main cause of deep vein thrombosis?
Ans:The primary cause of deep vein thrombosis is reduced or slowed blood flow, most commonly due to prolonged immobility, such as long travel or bed rest. When circulation slows, blood can pool and clot more easily. Surgery, injury, hormonal therapy, smoking, obesity, and certain medical conditions also increase risk.
What are the warning signs of deep vein thrombosis?
Ans:Warning signs often include swelling in one leg, calf pain or tenderness, warmth, redness, and a feeling of heaviness. Symptoms may develop gradually or suddenly. In some cases, DVT causes no obvious signs. Sudden shortness of breath or chest pain may indicate a serious complication called pulmonary embolism.
How serious is a deep vein thrombosis?
Ans:Deep vein thrombosis is potentially life-threatening because a clot can break loose and travel to the lungs, causing a pulmonary embolism. Without treatment, DVT may also lead to long-term complications such as chronic swelling, discomfort, and skin changes. Early diagnosis and treatment significantly reduce these risks.
What can trigger thrombosis?
Ans:Thrombosis can be triggered by factors that slow blood flow or increase clotting tendency. These include prolonged sitting, surgery, trauma, pregnancy, hormone therapy, cancer, dehydration, and inherited clotting disorders. Smoking and obesity also raise the risk. Often, multiple contributing factors are involved rather than a single cause.
How long can you have deep vein thrombosis without knowing?
Ans:Some people may have deep vein thrombosis for days or even weeks without noticeable symptoms. This is sometimes referred to as silent DVT. In certain cases, the first sign may be a pulmonary embolism. Individuals with risk factors should remain alert and seek evaluation if symptoms appear.
How to check for deep vein thrombosis at home?
Ans:There is no reliable way to confirm deep vein thrombosis at home. While symptoms such as swelling, calf pain, or warmth may raise suspicion, only medical imaging such as an ultrasound can provide a definitive diagnosis. If DVT is suspected, prompt professional medical evaluation is essential.
What could be mistaken for deep vein thrombosis?
Ans:Conditions such as muscle strains, cellulitis, Baker’s cysts, superficial thrombophlebitis, or even minor injuries can mimic DVT symptoms. Because these conditions may also cause swelling and pain, proper medical testing is necessary to accurately distinguish DVT from other, less serious issues.
Is walking good for deep vein thrombosis?
Ans:Walking may help improve circulation and can be beneficial after treatment has begun, depending on your doctor’s guidance. However, before a diagnosis is confirmed, strenuous activity should be avoided. Always follow a healthcare provider’s recommendations regarding safe movement and physical activity levels.
What not to do with deep vein thrombosis?
Ans:Do not ignore symptoms or delay seeking medical care. Avoid massaging or applying deep pressure to the affected leg, as this may increase the risk of clot movement. Prolonged immobility should also be avoided once treatment begins, unless otherwise directed by a healthcare provider.
When to worry about deep vein thrombosis?
Ans:Seek immediate medical attention if you experience sudden leg swelling, persistent calf pain, chest pain, shortness of breath, a rapid heartbeat, or coughing up blood. These symptoms may signal a pulmonary embolism, a serious complication that requires urgent emergency care.